Cupping reversal in pediatric glaucoma may not predict improved ONH health and deserves further study. The preoperative ONH cup-to-disc ratio predicted the postoperative RNFL better than the postoperative "reversed and smaller" cup-to-disc ratio. Some eyes with IOP reduction and ONH cupping reversal show continued RNFL thinning postoperatively. Limitations include small numbers, few reliable Humphrey visual fields, and absent preoperative imaging (Group 2). Postoperative RNFL showed statistically significant linear correlation with preoperative (but not postoperative) cup-to-disc ratio. Two eyes had thin RNFL postoperatively despite healthy-appearing ONH. Group 2: Fourteen of 24 PCG eyes (58%) demonstrated cupping reversal, with preoperative vs postoperative mean IOP 36.1 ± 8.9 mm Hg vs 13.3 ± 2.1 mm Hg (P <. Humphrey visual fields (reliable in 2 of 3 eyes) showed no significant change. RNFL was stable in 4 of 5 eyes (all juvenile OAG), but thinned (Δ = -41 μm) in 1 eye with PCG. Group 1: Five of 9 eyes (56%) demonstrated cupping reversal, with preoperative vs postoperative mean IOP 34.2 ± 6.6 mm Hg vs 10.6 ± 4.1 mm Hg (P <. Of 80 cases, 9 eyes (9 children) met criteria for Group 1 24 eyes (19 children) met criteria for Group 2. Cupping evaluation was confirmed by masked glaucoma and neuro-ophthalmology specialists. Group 1 had preoperative and postoperative ONH photographs and OCT Group 2 had preoperative clinical ONH assessment and postoperative imaging. Sequential surgical cases of juvenile open-angle glaucoma (OAG) or primary congenital glaucoma (PCG) with sustained postoperative intraocular pressure (IOP) reduction. To identify optic nerve head (ONH) cupping reversal and associated optical coherence tomography (OCT) and Humphrey visual field changes in pediatric glaucoma. Conclusions The 3D computerâ€automated threshold Amsler grid test may demonstrate visual field abnormalities characteristic ofĬupping reversal in pediatric glaucoma-evaluation of the retinal nerve fiber layer and visual field.Įly, Amanda L El-Dairi, Mays A Freedman, Sharon F No visual field changes were detected in the control group. Constricted visual fields were shown in 29% of the eyes. 71% of the eyes demonstrated arcuate defects or a nasal step. 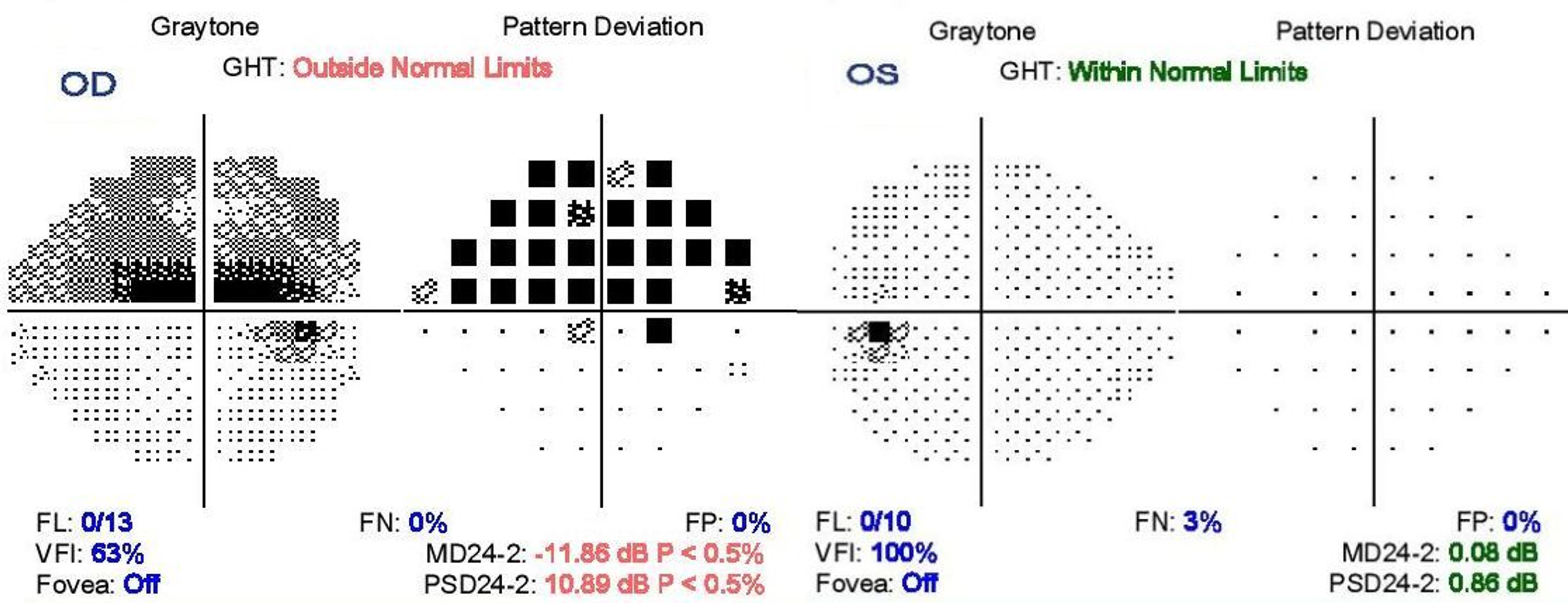
The 3D depictions of visual field loss associated with these risk factors were all characteristic of or compatible with glaucoma. Results In this pilot study 79% of the eyes tested in the glaucomaâ€suspect group repeatedly demonstrated visual field loss with the 3D perimetry. The results were compared to Humphrey visual field tests (ie, achromatic standard or SITA standard 30â€∂ or 24â€∂). The exam was repeated three times per eye. A 3D depiction of the visual field defects was then obtained that was further characterised by the location, shape and depth of the scotomas. The 5â€minute test required that the patients repeatedly outline scotomas on a touch screen with varied displays of contrast while maintaining their gaze on a central fixation marker. The test exhibits a grid on a computer screen at a preselected greyscale and angular resolution, and allows patients to trace those areas on the grid that are missing in their visual field using a touch screen. The recently developed 3D computerâ€automated threshold Amsler grid test was used. 15 patients and 23 eyes with no risk factors were tested as controls. 33 patients and 66 eyes with risk factors for glaucoma were examined. 
A χ2 test showed that the distributions of saccade directions for PVFL and FVL subjects were significantly different in 8 out of 10 cases (p 21 mm Hg) or cupâ€toâ€disc ratio of >0.5. High correlation coefficient ( r =0.808, P  0.1). The results were compared with those obtained from the same patients using the Humphrey perimeter. Virtual reality glasses, a smartphone with a 6 inch display, and software that implements a fast-threshold 3 dB step staircase algorithm for the central 24° of visual field (52 points) were used to test 20 eyes of 10 patients, who were tested in a random and consecutive order as they appeared in our glaucoma department. To present a visual field examination method using virtual reality glasses and evaluate the reliability of the method by comparing the results with those of the Humphrey perimeter. Tsapakis, Stylianos Papaconstantinou, Dimitrios Diagourtas, Andreas Droutsas, Konstantinos Andreanos, Konstantinos Moschos, Marilita M Brouzas, Dimitrios Visual field examination method using virtual reality glasses compared with the Humphrey perimeter. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
